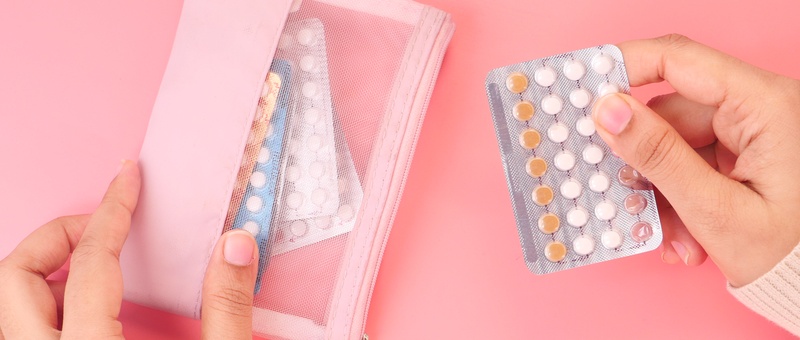
Qu'est-ce que le syndrome post-contraceptif ?
Revu par Dr Colin Tidy, MRCGPAuthored by Victoria RawPublié à l'origine 18 Jun 2025
Respecte les directives éditoriales
- TéléchargerTélécharger
- Partager
- Language
- Discussion
- Version audio
Après avoir arrêté la contraception, vous pouvez remarquer des changements physiques ou émotionnels dans votre corps. Bien que cela ne soit pas officiellement reconnu comme une affection médicale, ces symptômes sont souvent appelés le syndrome post-contraception (SPC).
Dans cet article:
Video picks for Contraception
There are many reasons you might choose to stop taking birth control - whether it's because you can no longer take it, no longer need it, or simply no longer want to.
Gérer le syndrome post-contraceptif - Symptômes et solutions
Debbie Grayson, Pharmacist and Nutritional Therapist, Practice With Confidence, Greater Manchester, UK explains that post-birth control syndrome (PBCS) refers to a collection of symptoms that some people have after discontinuing hormonal contraceptives.
"PBCS is not an officially recognised medical diagnosis, but the symptoms are real and can be distressing," she says. "They typically emerge within four to six months after stopping birth control."
Grayson outlines the most common PBCS symptoms:
Acné.
Irregular periods.
Sautes d'humeur.
Perte de cheveux.
You may experience breast tenderness, a decrease in sex drive, and weight gain - though this last symptom could be influenced by various factors unrelated to your birth control.
Continuez à lire ci-dessous
What causes post-birth control syndrome?
Most forms of birth control work to prevent pregnancy, by releasing synthetic hormones into your body that stop your ovaries from releasing eggs. If there is no egg to be fertilised, then sperm is unable to fertilise it during sex to make a baby.
There are eight types of birth control available in the UK, all of which are free through the NHS. You can access them via your doctor, sexual health clinics, or selected pharmacies.
Birth control options available in the UK
Combined pill - an oral contraceptive that contains both oestrogen and progestogen hormones.
Pilule progestative seule - an oral contraceptive commonly called the 'mini pill', that contains the hormone progestogen.
IUS (intrauterine system) - a small, plastic device, also called a 'hormonal coil', that releases progestogen into your womb.
Implant contraceptif - a small, plastic rod, inserted under the skin of your arm, that contains the hormone progestogen.
Injection contraceptive - an injection that contains the hormone progestogen.
Patch contraceptif - a square patch applied to your skin, that contains the hormone progestogen.
Vaginal ring - a small, plastic ring placed inside your vagina, that releases oestrogen and progestogen hormones.
IUD (intrauterine device) - a device, also known as a 'copper coil', that releases copper into your womb to stop sperm from surviving and fertilising an egg.
After you stop taking birth control, its effects typically disappear within about a month.
Grayson explains, however, that during this time, your body's hormone levels will take some time to adjust.
"This can lead to temporary disruptions," she explains. "Factors such as nutrient depletion, gut health, and hormonal detoxification play roles in this transition."
How is PBCS diagnosed and managed?
Retour au sommaireAs mentioned above, PBCS is not currently recognised as a health condition in the UK. As a result, you cannot seek a formal diagnosis from your doctor, even if you are having symptoms that may be related to it.
However, if you’re having symptoms such as irregular periods, mood swings, acne, fatigue, or digestive issues, it’s important to seek advice from a healthcare professional.
Grayson explains that there are several supportive strategies you can focus on to help restore your body’s natural balance and processes.
Top up on nutrients
Research suggests that hormonal contraceptives may deplete essential nutrients - such as B vitamins, magnesium, zinc, and vitamin C. Replenishing these through a balanced diet or targeted supplements can support your energy levels, mood, and overall hormonal health.
Boost your hormonal balance
Supporting your body’s natural hormone production is key to overall wellbeing.
According to Grayson, you can nurture your hormonal balance by:
Fuelling your body with a nutrient-rich diet - including healthy fats such as omega-3s, plenty of fibre, and quality protein.
Gérer le stress - through mindfulness practices, une bonne hygiène de sommeil, and regular exercise.
Minimising exposure to hormone-disrupting chemicals - by choosing safer skincare, avoiding plastic containers, and using non-toxic household products.
Keep your gut healthy
The health of your gut plays a crucial role in hormone metabolism and detoxification. Maintaining a healthy gut microbiome can help reduce symptoms such as bloating, acne, and mood swings.
This can be supported by:
Eating probiotic-rich foods - such as yoghurt, kimchi, and kefir.
Increasing your fibre intake.
Avoiding processed foods and excess sugar.
Grayson recommends checking in with a healthcare professional for personalised guidance after stopping birth control.
If you choose to come off it, it's important to tell your doctor so they can support you through the transition and help manage any after-effects.
Continuez à lire ci-dessous
How long does post-birth control syndrome last?
Retour au sommaireIt can take up to three months for your body to adjust after stopping birth control, and irregular periods during this time are common. However, if your menstrual cycle hasn’t settled after three months or if you’re having symptoms that interfere with daily life - such as painful or heavy periods - it’s important to speak with your doctor. They can offer tailored advice, support and, in some cases, may perform clinical tests or physical examinations to identify the underlying cause of your symptoms.
Patient picks for Contraception

Santé sexuelle
Quels médicaments peuvent affecter votre contraception ?
Certains médicaments, tels que les traitements contre l'épilepsie et le VIH, sont connus pour réduire l'efficacité des contraceptifs hormonaux. Cependant, il existe un débat sur la question de savoir si d'autres médicaments, comme les antibiotiques, peuvent également poser des problèmes de contraception. Nous examinons les dernières recherches.
par Natalie Healey
Santé sexuelle
Les pilules contraceptives modifient-elles votre comportement ?
La pilule contraceptive, en donnant aux femmes la possibilité de choisir si ou quand elles veulent tomber enceintes, offre à des millions de femmes une protection fiable mais réversible. En permettant aux femmes de modifier leurs hormones sexuelles, les pilules contraceptives peuvent leur donner le contrôle de leur corps. Cependant, il est important de savoir que la modification de ces hormones peut avoir des effets qui vont au-delà de la fertilité.
par Amberley Davis
Continuez à lire ci-dessous
Historique de l'article
Les informations sur cette page sont examinées par des cliniciens qualifiés.
Next review due: 19 Jun 2028
18 Jun 2025 | Publié à l'origine
Écrit par :
Victoria RawRevu par
Dr Colin Tidy, MRCGP

Demandez, partagez, connectez-vous.
Parcourez les discussions, posez des questions et partagez vos expériences sur des centaines de sujets de santé.

Vous ne vous sentez pas bien ?
Évaluez vos symptômes en ligne gratuitement
Inscrivez-vous à la newsletter Patient
Votre dose hebdomadaire de conseils de santé clairs et fiables - rédigés pour vous aider à vous sentir informé, confiant et maître de la situation.
By subscribing you accept our Politique de confidentialité. Vous pouvez vous désabonner à tout moment. Nous ne vendons jamais vos données.