Chéloïde
Revu par Dr Rosalyn Adleman, MRCGPDernière mise à jour par Dr Caroline Wiggins, MRCGP Dernière mise à jour 1 juil. 2025
Respecte les directives éditoriales
- TéléchargerTélécharger
- Partager
- Language
- Discussion
- Version audio
Un chéloïde (également appelé cicatrice chéloïde) est une prolifération excessive d'une cicatrice, après que la peau a été endommagée. C'est un type anormal de cicatrisation. Il est particulièrement fréquent chez les personnes à la peau foncée ou qui ont des membres de leur famille ayant développé des cicatrices chéloïdes.
Dans cet article:
Sélections de vidéos pour Autres problèmes de peau
Continuez à lire ci-dessous
What is a keloid scar?
A keloid scar is an overgrowth of the scar tissue that develops after a wound has healed. It expands beyond the original scar. Rather than stay in a straight line, for example, after a surgical incision, it can spread outwards and also upwards, giving a raised scar.
Who gets keloid scars?
Retour au sommaireKeloid scars are more common in people with black or brown skin, or white skin that tans after sunburn. Most people who develop a keloid are between 10-30 years old. Half of people with keloids will have members of their family who have also developed keloids.
Continuez à lire ci-dessous
What causes keloid scars?
Retour au sommaireWe don't yet have a definite answer to explain why some people go on to develop keloid scars after an injury. But we have a pretty good idea of how it happens.
Keloid scars are an overgrowth of scar tissue after a skin injury. The keloid becomes larger than the original wound. When a keloid scar is formed, we know that the process of normal scar tissue being created and gradually fading away, to reveal new, healed skin, is changed. There are many ideas being researched about why this may happen, but at the moment we don't know exactly why.
How does a keloid scar form?
Retour au sommaireKeloid scars typically starts to develop about three months after the original skin injury though it can occur years later. The first thing you will probably notice is that rubbery scar tissue starts growing beyond the borders of the original injury. The growth is usually slow and once they stop growing they usually stay the same size or they can get a bit smaller.
Typical areas keloid scars develop
Keloid scars occur most often on areas of the body where the skin is stretched, rather than where skin feels looser. They are more common on the upper body, for example:
On the ears, after ear piercing.
On the chest or back after chickenpox, acne, or an injury.
On the upper arms or shoulder.
If a keloid scar is over a joint, such as your elbow, it can restrict your ability to move that joint.
Continuez à lire ci-dessous
What do keloid scars feel like?
Retour au sommaireThey are usually smooth, slightly shiny, raised, firm skin growths which extend beyond the original skin injury.
They can feel itchy, prickly or sore.
Many people do not notice any itching or pain.
What do keloid scars look like?
Retour au sommaireThe image below shows a woman's ear affected by keloid scarring:
Keloid scarring on ear
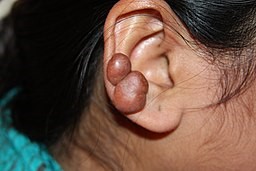
© Htirgan (Own work), CC BY-SA 3.0, via Wikimedia Commons
How does a doctor diagnose a keloid scar?
Retour au sommaireThere is no particular test for a keloid scar. It is diagnosed by a healthcare professional who will listen to what has happened, ask questions and examine the scar. They may want to look at scars you have elsewhere on your body to compare if this one is different to other ones you have.
Occasionally a keloid scar can mimic other skin tumours.
In that case, a biopsy will need to be taken by a specialist. A biopsie is a procedure where a sample of tissue is taken for further analysis.
The biopsy will be looked at under a microscope and a specialist (histopathologist) will be able to see the typical microscopic features of a keloid scar.
Remarque: a biopsy is hardly ever necessary because the history - that is, the patient's story - and the appearance of the skin growth allow the healthcare professional to diagnose a keloid without this test.
How to treat keloid scars
Retour au sommaireMany patients ask for their keloid scar to be 'cut out' (surgically excised). This is hardly ever successful and in fact can result in an even bigger keloid scar coming back. If surgical excision is tried it must be done by a specialist doctor such as a dermatologist or plastic surgeon and will usually be done in combination with another treatment.
Keloid scars can be difficult to treat and treatments can have side effects. It is important to be clear what you would like to achieve with treatment. Some people they want the itch or pain to improve, others want it to look more like the skin around the keloid. The medical team can then consider what treatment options are most likely to achieve what is important to you.
How to reduce keloid scars without surgery
One of the most common methods is injecting steroid (triamcinolone acetonide) and local anaesthetic into the keloid scar itself. The injections are done with a tiny needle, but can be a bit sore. This is called 'intralesional corticosteroid injection treatment':
The steroids and anaesthetic can help to stop the proliferation of the skin cells in the keloid scar.
The injections are usually given once a month for 4-6 months.
Side-effects of the steroids include the skin becoming thin, easily damaged, changing colour to become darker (hyperpigmentation) or lighter (hypopigmentation) than the surrounding skin, or being able to see many tiny blood vessels in the thinned skin.
New research suggests that combining the steroid injections with another form of treatment may reduce the possible side effects from the steroids and still improve the keloid. Many of these options are very new and the research is in small numbers of people and can give conflicting results. Further research is recommended before they are offered as standard treatments.
Other injection options may now include 5-FU, bleomycin, verapamil, hyaluronic acid and hyaluronidase, botulinum toxin, and collagenase.
Other treatment options include cryotherapy (using freezing temperatures), laser, radiofrequency ablation, radiation, and shock-wave therapy.
Sometimes steroids can be applied to the skin as an ointment under a dressing, or in a tape impregnated with steroids. can dampen down a keloid scar. Silicone dressings and compression dressings are also areas of research which have suggested they may help.
How to prevent keloid scars
Retour au sommaireIf you have a keloid scar then it is more likely future skin injuries will develop into a keloid scar. The best way to stop more keloids developing is to prevent unnecessary skin injuries.
People who are prone to keloid scars are advised to avoid body piercings, tattoos and ideally any surgery unless essential. Steer clear too of unnecessary procedures such as cosmetic surgery, especially in those areas of the body that are prone to keloids.
If you get acne, seek effective treatment at an early stage so the spots do not scar. If you are identified as being at risk of keloid and need an operation, your surgeon may offer you dressings, steroid injections or other treatments to reduce the risk of keloid developing.
Sélections de patients pour Autres problèmes de peau

Santé de la peau, des ongles et des cheveux
Albinisme
Albinism is a rare inherited (genetic) condition which reduces the amount of of melanin pigment in the skin, hair and/or eyes. People with albinism are often pale, with light-coloured irises. However, there are many types of albinism and people can be affected to different degrees.
par Dr Hayley Willacy, FRCGP

Santé de la peau, des ongles et des cheveux
Cors et callosités
Les cors et callosités sur les pieds sont des zones de peau épaissie qui peuvent devenir douloureuses. Ils sont causés par une pression excessive ou un frottement (friction) sur la peau et peuvent entraîner des problèmes de pieds, surtout en marchant. La cause courante est le port de chaussures mal ajustées. Une personne qualifiée pour diagnostiquer et traiter les troubles du pied (un podologue) peut enlever (parer) les cors et callosités et peut conseiller sur les chaussures, les semelles et les protections pour prévenir les récidives.
par Dr Colin Tidy, MRCGP
Lectures complémentaires et références
- Davidson S, Aziz N, Rashid RM, et al; A primary care perspective on keloids. Medscape J Med. 2009;11(1):18. Epub 2009 Jan 20.
- Limmer EE, Glass DA 2nd; A Review of Current Keloid Management: Mainstay Monotherapies and Emerging Approaches. Dermatol Ther (Heidelb). 2020 Oct;10(5):931-948. doi: 10.1007/s13555-020-00427-2. Epub 2020 Jul 23.
- Thornton NJ, Garcia BA, Hoyer P, et al; Keloid Scars: An Updated Review of Combination Therapies. Cureus. 2021 Jan 30;13(1):e12999. doi: 10.7759/cureus.12999.
- Keloid and hypertrophic scar; DermNet.
- Ekstein SF, Wyles SP, Moran SL, et al; Keloids: a review of therapeutic management. Int J Dermatol. 2021 Jun;60(6):661-671. doi: 10.1111/ijd.15159. Epub 2020 Sep 9.
Continuez à lire ci-dessous
Historique de l'article
Les informations sur cette page sont rédigées et examinées par des cliniciens qualifiés.
Prochaine révision prévue : 30 juin 2028
1 juil. 2025 | Dernière version
25 May 2011 | Publié à l'origine
Écrit par :
Dr Laurence Knott

Demandez, partagez, connectez-vous.
Parcourez les discussions, posez des questions et partagez vos expériences sur des centaines de sujets de santé.

Vous ne vous sentez pas bien ?
Évaluez vos symptômes en ligne gratuitement
Inscrivez-vous à la newsletter Patient
Votre dose hebdomadaire de conseils de santé clairs et fiables - rédigés pour vous aider à vous sentir informé, confiant et maître de la situation.
En vous abonnant, vous acceptez notre Politique de confidentialité. Vous pouvez vous désabonner à tout moment. Nous ne vendons jamais vos données.