Hypoglycémie
Hypoglycémie
Revu par Dr Toni Hazell, MRCGPDernière mise à jour par Dr Colin Tidy, MRCGPLast updated 9 sept. 2024
Respecte les directives éditoriales
- TéléchargerTélécharger
- Partager
- Language
- Discussion
- Version audio
Low blood sugar (hypoglycaemia) is often known as a 'hypo'. It can make you feel unwell and affect your ability to drive. Simple steps will reduce the risk, and allow you to treat a hypo early, before it causes more serious complications.
Inscrivez-vous à notre cours gratuit de 10 semaines sur le diabète !
Chaque semaine, nous explorerons un sujet différent pour vous aider à mieux comprendre et gérer votre diabète, y compris la vie quotidienne et les médicaments, le bien-être mental, les dernières technologies en matière de diabète et la nutrition.
By subscribing you accept our Politique de confidentialité. Vous pouvez vous désabonner à tout moment. Nous ne vendons jamais vos données.
Dans cet article:
Continuez à lire ci-dessous
Blood sugar - what's normal?
Under normal circumstances, your body does a remarkable job of keeping your blood sugar (in the form of glucose) stable. Usually your body releases a hormone called insulin, produced by your pancreas, in response to rises in blood sugar. Your body's cells need glucose as fuel to allow them to function. Insulin acts as a 'key', opening the door of your cells to allow in glucose. Another hormone helps raise your blood sugar if it gets too low.
Your blood sugar, which is measured in millimoles per litre (mmol/L) is usually maintained between 4 and 6 mmol/L when you're fasting, and up to 7.8 mmol/L two hours after a meal. Diabetes is diagnosed on the basis of raised blood glucose.
What causes hypoglycaemia?
Retour au sommairePeople with diabète de type 1 need de l'insuline in injection form, because they don't produce any insulin of their own. People with diabète de type 2 sometimes need insulin if their blood sugar can't be controlled with other tablets. If you're using insulin injections, the amount of insulin you need depends on lots of factors, including how much food you've eaten. More insulin than you need can drop your blood sugar below normal levels, causing a 'hypo'.
So too can some tablets used in type 2 diabetes, particularly les sulfonylurées, nateglinide and repaglinide, which act by making your body produce more insulin.
Hypoglycaemia is much less common in people without diabetes. The possible causes include:
Drinking excessive alcohol.
Some critical illnesses, eg, severe liver disease, infection, kidney disease, and heart disease.
Long-term starvation.
Insulin overproduction, eg, a rare tumour of the pancreas called an insulinoma.
Some hormone deficiencies, eg, certain rare adrenal gland and pituitary gland tumours.
Continuez à lire ci-dessous
Symptoms of hypoglycaemia
Retour au sommaireIf your blood sugar drops below about 4 mmol/L, you may experience:
Feeling weak or tired and hungry.
Feeling shaky and sweaty, with cold, clammy skin.
Irritability and poor concentration.
Headache and feeling sick.
Palpitations.
Vision floue.
If your blood sugar continues to drop, you may develop:
Confusion and drowsiness.
Poor co-ordination.
Difficulty speaking.
Irrational behaviour.
Collapse and loss of consciousness.
In very severe cases, hypoglycaemia can be fatal.
How to prevent hypoglycaemia
Retour au sommaireIf you have type 1 diabetes, you'll often be encouraged to control your blood sugar to almost the same levels as someone who doesn't have diabetes, especially if you're young and don't have complications of diabetes or other medical conditions. This is because high blood glucose in the long term is linked to damage to your reins, eyes, nerves, feet and heart. However, keeping tight control of your blood glucose does increase the risk of hypos.
Reducing the risk of hypos
Having said that, there are lots of steps you can take to reduce the risk of hypos. These include:
Not skipping or delaying snacks or meals.
Learning about the right dose of insulin you need for a given amount of carbohydrate.
Adjusting your insulin if you're exercising vigorously.
Avoiding alcohol, and particularly drinking on an empty stomach.
Speaking to your medical team in advance of situations where your normal eating will be disrupted (eg, at Ramadan, or if you're travelling or working shifts) so you can work together to adjust your insulin dose.
If you're taking sulfonylurea tablets and getting symptoms that you think may be hypos, speak with your team. They may be able to change your medication, as there are many alternative treatments for type 2 diabetes that don't cause hypos.
Keeping a supply of sugary drink, fruit juice or glucose tablets to hand at all times, so you can treat symptoms early.
Checking your blood glucose regularly.
Flash glucose monitors (Freestyle Libre) and continuous glucose monitors (CGM)
Flash glucose monitors and continuous glucose monitors let you check your sugar levels without having to prick your fingers. A small sensor on your body reads your sugar levels so you can see the information on your mobile, or other device. If someone helps you look after your diabetes, their mobile can be linked up too. Both a CGM and a flash glucose monitor (FreeStyle Libre2) also let you set an alarm to sound if your sugar levels go too low or too high.
Flash glucose monitors and CGMs allow you to review your sugar levels every minute of the day and night. This helps you understand how food and activity affect your sugar levels.
Continuez à lire ci-dessous
How often should I check my blood sugar?
Retour au sommaireNot everyone with type 2 diabetes needs to check their own blood glucose - it's usually recommended only if you're taking insulin injections, or some other Type 2 diabetes medicines, such as a sulfonylurea; if this isn't the case, your GP will not prescribe strips and lancets to check blood sugar, as this isn't necessary. Obviously you still need to attend for regular diabetes checks, where your blood sugar and HbA1c will be monitored. HbA1c is a measure of your average blood glucose control over the previous three months.
If you have type 1 diabetes, you should always check your blood sugar regularly. Your doctor or nurse will usually recommend that you check at least four times a day, including before each meal and before bed, even if you're not driving.
If you're driving and taking insulin or other medication that could cause hypos, the DVLA recommends that you should check your blood glucose less than two hours before you start driving and every two hours while you are driving.
What should I do if my blood sugar is low?
Retour au sommaireA 'hypo' is usually defined as a blood glucose below 4 mmol/L. A useful way to remember it is 'Five, don't drive; four is the floor'. In other words, if your blood glucose is below 5 mmol/L, you shouldn't drive. If it's below 4 or you have symptoms of a hypo:
Stop what you're doing (pull over as soon as it's safe if you're driving and take the keys out of the ignition).
Check your blood glucose if you haven't already.
Immediately eat some glucose tablets or sugary sweets (jelly babies are ideal) or drink fruit juice or a sugary drink - the standard recommended amount is 15-20 grams of fast-acting carbohydrate.
Warn anyone you're with about what's happening, so they can help if your symptoms get worse.
Relax for 15 minutes or so while your blood glucose rises.
Check your blood glucose again. Don't drive until at least 45 minutes after it has risen above 5 mmol/L.
You may also need to eat another snack, or a meal if it's due - your medical team can advise.
How can I help if I think someone is having a hypo?
Retour au sommaireThe symptoms of hypos can often be mistaken for drunkenness. So if you see someone acting oddly, especially if you know or suspect they have diabetes, check if they have:
A medical alert bracelet or similar.
An insulin pen or syringe, or glucose testing kit.
Glucose gel or sugary sweets.
Then:
Help them sit down quietly.
If they have their own glucose gel, help them take it.
Otherwise, give them sugary sweets, two teaspoons of sugar, or a glass of sugary drink or fruit juice (even if you're not sure they're having a hypo, it's safer to do this).
Keep a careful eye on their level of responsiveness, breathing and pulse.
If they get better, make sure they check their blood glucose.
If they don't improve, call 999 (if in the UK).
Patient picks for Vivre avec le diabète

Diabète
Ulcères du pied diabétique
Certaines personnes atteintes de diabète développent des ulcères du pied, en raison d'une mauvaise circulation sanguine et d'une sensibilité réduite dans les pieds. Un examen régulier des pieds et un bon contrôle du diabète aident à les prévenir. Un ulcère du pied est sujet à l'infection, qui peut devenir grave. Les ulcères nécessitent parfois un traitement avec des pansements, des médicaments et, le cas échéant, une intervention chirurgicale.
par Dr Colin Tidy, MRCGP
Diabète
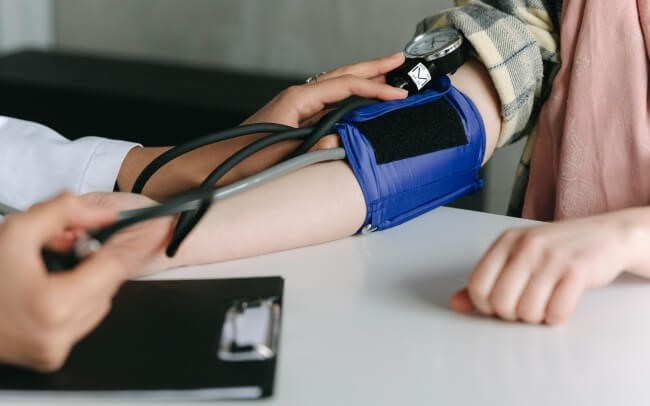
Diabète et hypertension artérielle
Il est important de maintenir votre tension artérielle sous contrôle si vous avez du diabète. Les AVC, les maladies cardiaques et d'autres complications sont plus probables si votre tension artérielle est élevée. S'attaquer aux facteurs malsains de votre mode de vie peut aider. Certaines personnes ont besoin de médicaments si les changements de mode de vie ne suffisent pas.
par Dr Doug McKechnie, MRCGP
Inscrivez-vous à notre cours gratuit de 10 semaines sur le diabète !
Chaque semaine, nous explorerons un sujet différent pour vous aider à mieux comprendre et gérer votre diabète, y compris la vie quotidienne et les médicaments, le bien-être mental, les dernières technologies en matière de diabète et la nutrition.
By subscribing you accept our Politique de confidentialité. Vous pouvez vous désabonner à tout moment. Nous ne vendons jamais vos données.
Lectures complémentaires et références
- Diabetes UK
- Iqbal A, Heller S; Managing hypoglycaemia. Best Pract Res Clin Endocrinol Metab. 2016 Jun;30(3):413-30. doi: 10.1016/j.beem.2016.06.004. Epub 2016 Jun 14.
- Diabète de type 1 chez les adultes : diagnostic et gestion; Directives NICE (août 2015 - dernière mise à jour août 2022)
- Diabète (type 1 et type 2) chez les enfants et les jeunes : diagnostic et prise en charge; Directives NICE (août 2015 - mis à jour mai 2023)
- Diabète de type 2 chez les adultes : gestion; Recommandations NICE (décembre 2015 - dernière mise à jour juin 2022)
Historique de l'article
Les informations sur cette page sont rédigées et examinées par des cliniciens qualifiés.
Prochaine révision prévue : 8 sept. 2027
9 sept. 2024 | Dernière version

Demandez, partagez, connectez-vous.
Parcourez les discussions, posez des questions et partagez vos expériences sur des centaines de sujets de santé.

Vous ne vous sentez pas bien ?
Évaluez vos symptômes en ligne gratuitement
Inscrivez-vous à la newsletter Patient
Votre dose hebdomadaire de conseils de santé clairs et fiables - rédigés pour vous aider à vous sentir informé, confiant et maître de la situation.
By subscribing you accept our Politique de confidentialité. Vous pouvez vous désabonner à tout moment. Nous ne vendons jamais vos données.