Plaies infectées
Revu par Dr Toni Hazell, MRCGPDernière mise à jour par Dr Philippa Vincent, MRCGPLast updated 7 oct. 2024
Respecte les directives éditoriales
- TéléchargerTélécharger
- Partager
- Language
- Discussion
- Version audio
Dans cette série :Fasciite nécrosante
Une infection peut survenir sur tout type de blessure - qu'il s'agisse d'une petite coupure, d'une intervention chirurgicale ou d'une blessure accidentelle. Les signes qu'une plaie est infectée comprennent une douleur qui s'aggrave, un gonflement, une rougeur qui s'étend, une chaleur accrue autour de la plaie et du pus. Cette brochure aborde les symptômes à surveiller, les traitements et le moment de consulter un médecin.
Dans cet article:
Video picks for Infections cutanées
Points clés
An infected wound happens when bacteria enters a cut, graze, surgical wound, or bite.
Signs a wound is infected include pain, redness that spreads, swelling, skin that is warm to touch, and pus.
Symptoms such as fever, having general aches and pains, or feeling generally unwell may indicate sepsis, and requires urgent medical care.
Mild infections may heal with good wound care, while more serious ones might need antibiotics or surgical cleaning.
Continuez à lire ci-dessous
How to tell if a wound is infected
The body is usually very good at healing wounds. Wound healing requires inflammation: the body activates the immune system to repair damage, and so inflammation is a good thing at the beginning of wound healing.
Sometimes wounds can become infected, which might make them slower to heal, or cause other problems, such as a serious infection that spreads.
The body reacts to infection by producing more inflammation. So, an infected wound might have signs of too much inflammation.
Infected wound
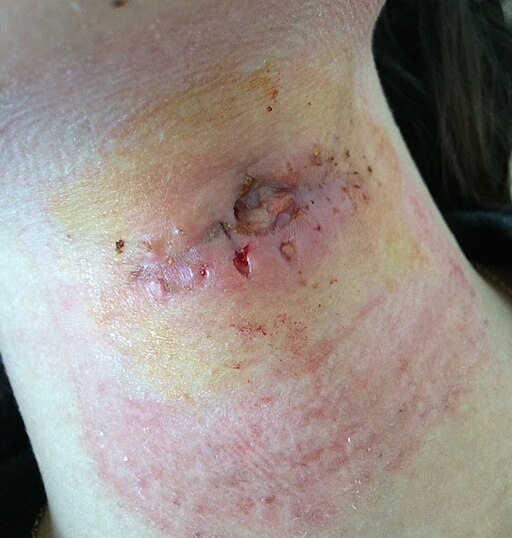
© Bp20151130, CC BY-SA 4.0, via Wikimedia Commons
How to know if a wound is healing or infected
Signs that a wound is healing normally include:
The wound scabbing over.
Mild redness or swelling around the wound (this is normal, and helpful, inflammation).
Pink or red tissue at the bottom of the wound (called 'granulation tissue' - an important stage of healing).
Mild warmth over the wound, which improves over time.
Mild pain or discomfort which is improving over time.
The wound gradually improving.
Scar tissue developing (this is one of the last parts of wound healing).
Signs that a wound is infected include:
Worsening pain at the site of the wound.
Lots of swelling at the site of the wound.
Discharge from the wound, particularly if pus is coming out of the wound (yellow-white liquid).
The wound, or skin around it, feeling hot to touch.
Redness that is spreading across the skin around the wound.
Other signs of infection in the body, like having a fièvre, having general aches and pains, or feeling generally unwell.
Having these symptoms may indicate a serious infection, such as septicémie.
It can sometimes be difficult to tell if a wound is infected so medical advice should be sought if unsure.
What to do if a wound is infected
Retour au sommaireSurgical wound infection
If you think a cut from an operation (a surgical wound) is infected, you should speak to a healthcare professional as soon as possible. It's best to contact the team who did the operation directly as they are responsible for all post-operative care as well. If that's not possible, it may be necessary to attend an urgent care centre or even the accident and emergency department.
A healthcare professional should ask a few questions and then examine the wound to determine if it's infected or not.
If they think it's infected, they might take a swab of the wound and any discharge. This is sent to a laboratory to find out which bacteria are causing the infection, and which antibiotics work against them. It takes several days for the result to come back.
Sometimes, if a more serious infection is suspected, blood tests and scans might be needed. These are usually done in hospital.
Trauma wound infection
With a laceration, cut or graze, keep an eye on it. You should:
Keep it clean by bathing it with warm water and clean cotton wool.
Try an antiseptic cream, such as Savlon®.
If the redness is spreading or the wound starts to ooze pus, seek medical advice.
If it is a larger wound and seems to be developing infection, then see your doctor or nurse straight away.
Continuez à lire ci-dessous
How do you treat an infected wound?
Retour au sommaireTreatments for an infected wound include:
No treatment: the body is usually good at fighting off minor infections, and mild wound infections can often be monitored to see if they get better on their own.
Wound care: cleaning the wound every few days and applying sterile (clean) wound dressings. Some types of wound dressing are anti-bacterial.
Antibiotic creams: creams such as acide fusidique can be used on minor wound infections.
Antibiotic capsules and tablets: these are likely to be needed for large wound infections, major infections, infections which are getting worse, and infections that are likely to get worse without treatment (such as surgical wound infections).
For severe wound infections, hospital treatment may be required:
Antibiotics may need to be given intravenously (through a drip) for serious wound infections.
Serious infections may require an operation ('debridement') to remove infected and dead tissue from the wound.
Do I need a tetanus injection?
Retour au sommaireTetanus is a serious disease caused by germs which mostly live in soil or manure. Wounds which have been in contact with soil or manure, or which are particularly 'dirty', may increase the risk of developing tetanus. Tetanus is rare in the UK, because most people are protected from tetanus by vaccinations.
If you're fully up-to-date with your tetanus vaccines (you've had at least 3 vaccines, and the last vaccine was given less than 10 years ago), you don't need another vaccine after a wound.
If you've had at least 3 tetanus vaccines, but the last vaccine was given more than 10 years ago, you only need another tetanus vaccination if the wound is 'dirty' (eg, soil or dirt is in the wound). For a clean wound, you don't need another vaccination.
If you've never had the full initial course of tetanus vaccines (3 injections), you should have a tetanus vaccine after any wound, even if it's a 'clean' one.
Tetanus vaccines can be given by a nurse in a general practice surgery, or in the Emergency Department.
Continuez à lire ci-dessous
Why do wounds get infected?
Retour au sommaireWounds heal best when they are clean and free from germs. Normally, many bacteria live harmlessly on our skin and in the environment around us. Normally the bacteria live on our skin, or in areas such as our nose, without causing any problems.
Usually the skin acts as a barrier. If the skin is broken, bacteria may spread into the more sensitive tissues underneath. This is how an infection can start. This makes the tissues sore and swollen, and less likely to heal. Open wounds are more likely than closed wounds to develop infections because the break in the skin provides a route for the germs to travel from the outside to the inside.
Some circumstances make it more likely that wounds will become infected. These include:
Having diabetes (type 1 ou type 2).
If the object which caused the wound was dirty and contained germs.
If the wound was caused by a human or animal bite. (Human and animal mouths contain lots of bacteria, and bites can make deep holes in the skin.)
If the wound still contains a 'foreign body', ie bits of whatever caused the injury, for example, bits of glass, splinters of wood, thorns, etc.
The size and depth of the wound. Larger or deeper wounds have a higher chance of becoming infected.
Jagged edges to the wound.
If proper precautions were not taken before an operation.
In older people. Skin heals less well as you get older.
In people who are very overweight. In skin folds, retained moisture can encourage the growth of bacteria and fungi.
If the immune system does not work as well as normal, for example, in people on medication such as stéroïdes ou chemotherapy, or who are on immunosuppressant medication for conditions like rheumatoid arthritis and inflammatory bowel disease, or who have untreated HIV/AIDS.
Are wound infections dangerous?
Retour au sommaireMild infections of small, shallow wounds can heal on their own, particularly in healthy people.
Sometimes, wound infections can spread and cause serious problems. This is more likely with large wounds, deep wounds, and surgical wounds, and in people who are more vulnerable to infection.
If a wound infection spreads, it can cause infection of the deep tissues under the skin (la cellulite). A severe wound infection may cause bacteria to enter the bloodstream, causing septicémie - which can be life-threatening.
If you have a wound and start to feel unwell in yourself, it is very important to know the signs of possible septicémie. Sepsis is always a medical emergency - if you have any concern that you might be developing sepsis, seek immediate medical help. See the sepsis leaflet for more information.
Other possible complications include:
The wound may heal less well if it is infected.
Other types of skin infection may develop such as impetigo.
It can turn into a painful lump of pus called an abscess.
Very rare complications include:
Developing a further infection with tétanos. This is very rare in the UK, because most people are vaccinated against it.
Developing a further infection called necrotising fasciitis. Necrotising fasciitis is sometimes called 'flesh-eating disease'. In necrotising fasciitis, bacteria aggressively spread rapidly through the body, starting from the wound. It is very rare, but can be life-threatening.
How can I prevent wound infection?
Retour au sommaireWound infection can largely be prevented by keeping the area clean.
Preventing infection in surgical wounds
During an operation the surgical team has strict procedures to try to help avoid infections. Surgical infections are monitored by the UK Health Security Agency so that policies can be changed and improved if needed.
There are a number of things that can be done by individuals to reduce the chance of infection. For example:
Have a shower or bath before the operation and wash with soap and water.
Do not use a razor to shave the area to be operated on as this makes infection more likely. If the hair needs to be removed, the surgical team will do this with clippers.
Remove all jewellery and nail polish before the operation.
Keep the wound covered and the area around it clean. Showering is usually possible from two days after most operations.
If the skin around the wound is becoming red or painful, medical advice should be sought.
Preventing infection in wounds from injuries
Tips to avoid infection of traumatic wounds:
Clean the wound and skin around it as soon as it happens. Use cool boiled water, or drinking-quality water.
If there are still bits of foreign bodies in the wound, go to the nearest Minor Injuries Unit or A&E to have it professionally cleaned out.
If it is a very deep wound, or the edges are very far apart, or the bleeding is not stopping, go to the nearest Minor Injuries Unit or A&E in case it needs stitches.
Use an antiseptic around the wound area to help keep the germs away.
Put a clean dressing over your wound to protect it from germs. Do not use gauze or a type of dressing which will stick to the wound. A pharmacist should be able to advise on the best dressing if the wound is too big for an ordinary plaster.
Human ou animal bites are very likely to become infected. Bites where the teeth have broken the skin are the one scenario where antibiotics are often given to prevent infections developing rather than waiting to see if an infection develops. Seek medical advice for a human or animal bite which has broken the skin.
Keep a close eye on the wound and seek medical advice infection appears to be developing.
Request a tetanus vaccination if needed.
Questions fréquemment posées
Retour au sommaireHow to know if a wound is septic?
If you have symptoms such as sudden confusion, feeling extremely unwell, difficulty breathing or breathing very fast, feeling cold or clammy, having pale or mottled skin, muscle pain, or blue, grey, or pale skin, lips or tongue, then you should seek medical help immediately as it could be a sign of sepsis.
Is saltwater good for infected wounds?
A sterile saline solution made up of cooled, boiled water and salt can help clean a wound and promote healing, but it isn’t a substitute for proper medical care. You should see a doctor or pharmacist if you have signs of an infected wound.
Can an infected wound cause nausea?
Severe infections can cause nausea alongside symptoms such as fever and chills. You should seek medical help if you have any of these symptoms.
How often should dressings be changed on an infected wound?
Dressings are usually changed once a day or when they become wet or dirty, but exactly how often depends on the type of wound and your doctor’s advice.
Patient picks for Infections cutanées

Infections
Furoncles, anthrax et furonculose
Un furoncle est une infection d'un follicule pileux. Un anthrax se produit lorsqu'un groupe de follicules pileux adjacents s'infecte. C'est comme un furoncle multiple. La furonculose chronique est une condition où vous avez des poussées de furoncles qui se produisent sur une période prolongée.
par Dr Colin Tidy, MRCGP

Infections
Varicelle chez les adultes et les adolescents
La varicelle provoque des boutons (une éruption cutanée) et peut vous faire sentir mal. Les symptômes ont tendance à être plus graves chez les adultes que chez les enfants. Les traitements peuvent soulager les symptômes jusqu'à ce que la maladie disparaisse. Un médicament antiviral peut limiter la gravité de la maladie si le médicament est commencé dans les 24 heures suivant l'apparition de l'éruption. Un rétablissement complet est habituel. Les complications graves sont rares, mais sont plus fréquentes chez les adultes que chez les enfants. Elles sont plus susceptibles de se produire chez les femmes enceintes et chez les personnes ayant un système immunitaire affaibli, comme celles sous chimiothérapie. Si vous êtes enceinte et n'avez pas eu la varicelle (ou n'avez pas été immunisée) et entrez en contact avec une personne atteinte de la varicelle - consultez votre médecin de toute urgence, car un traitement peut empêcher le développement de la varicelle.
par Dr Colin Tidy, MRCGP
Lectures complémentaires et références
- Surgical site infections: prevention and treatment; NICE guideline (April 2019 - last updated August 2020)
- Bites - human and animal; NICE CKS, août 2024 (accès réservé au Royaume-Uni)
- Lacerations; NICE CKS, décembre 2022 (accès réservé au Royaume-Uni)
Continuez à lire ci-dessous
Historique de l'article
Les informations sur cette page sont rédigées et examinées par des cliniciens qualifiés.
Prochaine révision prévue : 6 oct. 2027
7 oct. 2024 | Dernière version

Demandez, partagez, connectez-vous.
Parcourez les discussions, posez des questions et partagez vos expériences sur des centaines de sujets de santé.

Vous ne vous sentez pas bien ?
Évaluez vos symptômes en ligne gratuitement
Inscrivez-vous à la newsletter Patient
Votre dose hebdomadaire de conseils de santé clairs et fiables - rédigés pour vous aider à vous sentir informé, confiant et maître de la situation.
By subscribing you accept our Politique de confidentialité. Vous pouvez vous désabonner à tout moment. Nous ne vendons jamais vos données.