Atrial fibrillation and stroke prevention
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 19 Dec 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
In this series:Atrial fibrillation
The medicines used to prevent a atrial fibrillation-related stroke are called anticoagulants. These help to stop blood clots forming in your blood vessels.

Unsure about mixing medicines?
Check for possible interactions between medicines, supplements and foods before taking them together.
In this article:
Video picks for Heart and blood medicines
Continue reading below
Why does atrial fibrillation increase your risk of having a stroke?
The main complication of atrial fibrillation (AF) is an increased risk of having a stroke. AF can interfere with the blood flow in the heart chambers. This sometimes leads to a small blood clot forming in a heart chamber.
A clot can travel in the blood vessels until it becomes stuck in a smaller blood vessel in the brain (or sometimes in another part of the body). Part of the blood supply to the brain may then be cut off, which causes a stroke. Strokes due to AF tend to be even more serious than strokes due to other causes.
The risk of developing a blood clot and having a stroke varies, depending on several factors. The level of risk can be calculated by your doctor using a set of specific questions. This will help to decide what treatments are required. All people except those at the lowest risk will be offered medication to help prevent clots from forming.
How can the risk of stroke be reduced?
Back to contentsMedicines called anticoagulants can be used to reduce the risk of a blood clot and so reduce the risk of stroke. Anticoagulants work by prolonging the time it takes for blood to form a clot. Some people call anticoagulation 'thinning the blood', although the blood is not actually made any thinner.
Anticoagulants reduce the risk of stroke by nearly two thirds. In other words, these treatments can prevent about 6 out of 10 strokes that would have occurred in people with AF.
Continue reading below
Should you take medicine to reduce your risk of stroke?
Back to contentsYour doctor can use a risk assessment to see if you should take medicine to reduce your risk of stroke. The most commonly used risk assessment tool is called the CHA2DS2-VASc risk score. Points are added for each of the following it they apply to you:
Congestive heart failure with a recent exacerbation (1 point).
Hypertension - past or present (1 point).
Aged 75 years or older (2 points).
Diabetes (1 point).
Past history of a Stroke or transient ischaemic attack (2 points).
Vascular disease - for example, peripheral arterial disease, angina or previous heart attack (1 point).
Age 65-74 years (1 point).
Sex category (ie female sex scores 1 point and male scores 0).
The higher the total points score, the higher the risk of stroke. Everyone with a score of 2 or more should be treated with anticoagulation. Men with a risk of 1 may be offered anticoagulation. Women with a risk of 1 (in other words, where female sex is their only risk factor) are not offered anticoagulation because the benefits of treatment are likely to be outweighed by the risks.
Another risk score called the HAS-BLED score is used to estimate the risk of major bleeding when you are taking a medicine to reduce the risk of stroke if you have AF. This helps to decide whether or not steps should be taken to reduce your risk of bleeding if you take anticoagulation.
A risk score called ORBIT can be used to assess your risk of major bleeding, including bleeding into the brain. For most people, the benefit of anticoagulation outweighs the bleeding risk. However, if your bleeding risk is high and cannot be reduced, your doctor will discuss the pros and cons of starting (or stopping) anticoagulation.
The National Institute for Health and Care Excellence (NICE) advises that the ORBIT risk score should be used instead of HAS-BLED to assess the risk of major bleeding when starting blood-thinning medication and whilst you are on it. This is because the evidence shows that it has a higher accuracy in predicting the risk of bleeding than other bleeding risk tools.
The CHA2DS2-VASc stroke risk score and ORBIT bleeding risk score should be reassessed at least annually.
Which medicines help to reduce the risk of stroke?
Back to contentsAspirin is very effective at reducing the risk of a second stroke if you have had a stroke which was not due to AF. However, where AF-related stroke is concerned, aspirin is much less effective than other treatments but just as likely to cause problems. It is therefore no longer recommended to reduce the risk of stroke in AF.
Instead, your doctor is likely to recommend an anticoagulant. In the past, warfarin was the traditional option. However, several newer agents called direct-acting oral anticoagulants (DOACs) are now available. These are called:
Studies have shown the DOACs to be at least as effective as warfarin for reducing the risk of an AF-related stroke. In addition, they:
Carry a lower risk of bleeding into the brain.
Need much less frequent blood monitoring (you do not need regular INR blood clotting tests).
Have fewer interactions with other medications or food. These interactions could otherwise result in you being more prone to bleeding or clotting.
Do not require you to adjust the dose frequently dependent on your blood results, as warfarin does.
As a result, NICE has updated its guidance to recommend that DOACs should be offered in preference to warfarin. If you are already taking warfarin, your doctor may discuss changing you to treatment with a DOAC, depending on the results of your blood tests.
To find out more about these medicines, including the risks and benefits of the various alternatives, see the separate leaflet called Anticoagulants.
Continue reading below
Surgery
Back to contentsAn operation can be used to reduce the risk of stroke for people with AF. The operation is called left atrial appendage occlusion and closes a pouch in the heart, called the left atrial appendage.
NICE in the UK has recommended that left atrial appendage occlusion can be considered as a treatment option to reduce the risk of stroke in people with AF. However, it does carry risks. It is therefore reserved for people who are at high risk of stroke and who cannot take anticoagulants.
Patient picks for Heart and blood medicines
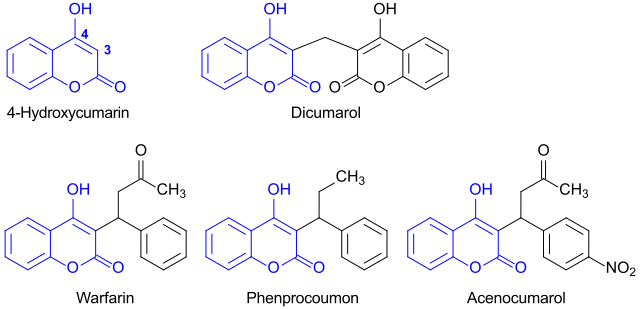
Treatment and medication
Anticoagulants
Anticoagulants are medicines that prevent the blood from clotting as quickly or as effectively as normal. Some people call anticoagulants blood thinners. However, the blood is not actually made any thinner - it just does not clot so easily whilst you take an anticoagulant. Anticoagulants are used to treat and prevent blood clots forming in blood vessels, such as in arteries or veins.
by Dr Doug McKechnie, MRCGP
Treatment and medication
Medicine for high blood pressure
For detailed information about your own medication you should read the leaflet that comes inside the medicine packet.
by Dr Philippa Vincent, MRCGP

Unsure about mixing medicines?
Check for possible interactions between medicines, supplements and foods before taking them together.
Further reading and references
- Atrial fibrillation: diagnosis and management; NICE guideline (April 2021 - last updated June 2021)
- Atrial fibrillation; NICE CKS, October 2024 (UK access only)
- Thoracoscopic exclusion of the left atrial appendage in atrial fibrillation (with or without other cardiac surgery) for the prevention of thromboembolism, NICE Interventional Procedure Guideline, June 2011
- WatchBP Home A for opportunistically detecting atrial fibrillation during diagnosis and monitoring of hypertension; NICE Medical Technologies Guidance, January 2013
- European Society of Cardiology; Guidelines for Management of Atrial Fibrillation, 2020
- Isaew A, Adderley NJ, Ryan R, et al; The treatment of paroxysmal atrial fibrillation in UK primary care. Heart. 2017 Jun 1. pii: heartjnl-2016-310927. doi: 10.1136/heartjnl-2016-310927.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 18 Dec 2027
19 Dec 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.